Opening Up About Prostate Cancer
Let’s hear it for the boys – men we love you but really need you to take this cancer thing much more seriously. Get checked!

I’m a boy mom. I’m wife to an amazing man. I’m also a little sister to a guy. I’m a little sister-in-law to two guys. I have my dad, father in law, uncles, and all my husband’s and brother’s friends. Its easy to say that I am surrounded by boys. I do have a girl dog though for good measure.
With Father’s Day just around the corner, I wanted to take some time to talk about a cancer that most men don’t want to mention, much less receive screening tests for. You guessed right – prostate cancer. Be advised that words such as rectum and erection are going to be used below, so if you blush easily, consider yourself warned.
Why don’t men get screened?
The American Cancer Society recommends that men begin discussing screenings for prostate cancer at about the age of 50, unless they are at a higher risk for developing disease. A recent article cited a study by the Cleveland Clinic that only 60% of men get annual physicals. Of those men surveyed – 19% admitted to only going to the doctor to get a loved one to stop nagging them. We ladies go in for yearly exams at the gynecologist at a seemingly higher rate – but why is that? The Cleveland Clinic study showed that men would rather talk about anything else but their health, whereas in my experience, women are much more verbal in that arena.
What are the screening tests?
There are two types of screening tests for prostate cancer – one is a blood test and the other is the digital rectal exam (DRE). The blood test looks at the levels of prostate stimulating antigen (PSA) in the blood. Cancer.org tells us that the average level for a healthy man with a healthy prostate is around 4, but that can vary. The DRE, on the other hand (no pun intended), is pretty self-explanatory. The prostate is a donut shaped organ that sits at the base of the bladder and surrounds the urethra; it can be felt through the wall of the rectum. With a DRE, the physician can feel for abnormalities in size, shape, and texture.
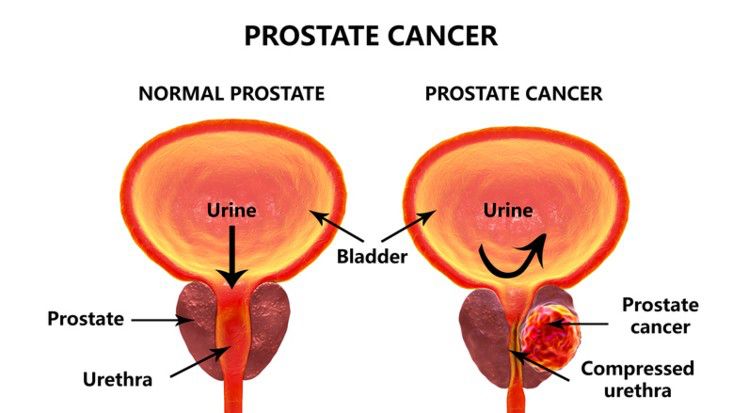
So, here’s the deal with these screening tests. While an elevated PSA can be indicative of cancer, just as an enlarged prostate, it can also be a sign of benign prostatic hyperplasia – or enlarged prostate – a condition that presents itself in 50% of men between the ages of 50 and 60. There are a host of other issues that can cause abnormal screening tests such as age, urinary tract infection, recent sexual activity, and injury. Be sure to discuss these with your physician before having a screening test so he or she can interpret your results with clarity.
If your physician is concerned about the results of a screening test, they will likely proceed by ordering a biopsy of the prostate itself. And you guessed correctly, they usually go in rectally. If a malignancy is found on the biopsy, they will be able to give you a lot more information on slow versus fast growth, aggressiveness of the disease, and treatment options.
You may be wondering if, given the chances of a false positive, it is worth having screenings. Honestly, that is between you and your doctor. I have seen a close family member have a scare with high PSA values, an abnormal DRE, and a perfectly normal biopsy. His best friend, however, with the same screening results, did have an prostatic carcinoma. They both believe that screening is worth it.
Risk factors
Above we spoke about getting screened earlier than 50 if you are at a higher risk. So, what are those risk factors? Below are a few from cancer.org:
- Age: 60% of prostate cancer cases are in men older than 65.
- Race: African-American men are at a much higher risk of prostate cancer, as well as Caribbean men of African descent.
- Geography: although it isn’t understood why, men living in North America, northwest Europe, Australia, and in the Caribbean are at a higher risk for the development of prostate cancer.
- Family history of the disease
Treatment options
If you or a loved one should be diagnosed with prostate cancer, there are a lot of options to consider, depending on factors such as how aggressive the type of cancer is, and also staging. These options can include radiation, chemotherapy, and surgery. Other non-standard treatment options such as cryotherapy and hormone therapy may be appropriate depending upon the case.
From talking to those men that I know who have dealt with prostate cancer, the two biggest concerns going into treatment are urinary incontinence and erectile issues. Cancer.org tells us that larger cancer centers, with surgeons that deal with these surgeries more often, report lower levels of incontinence in their patients, as well as the fact that these issues may resolve to some extent over time. The same holds true for sexual function. If the never bundles that control erection are able to be spared, sexual function may also be spared; however, if the cancer has invaded those nerves, erectile function will be affected. If this is an issue for you or a loved one, don’t be shy – discuss this with your urologist. There are pharmaceuticals and other therapies that may help restore function.
The latest
USA Today reported on June 4th of this year that a clinical trial in the UK involving Keytruda in men with otherwise untreatable prostate cancer was showing positive results. After one year, 38% of men in this dire population were still alive, and 5% had tumors that had shrunk or gone away! Keytruda is an immontherapy agent that is being tested in several indications. Please see Immunotherapy and Cancer for a glimpse at these amazing compounds, and our listing of Clinical Trials for more information on possibilities for you.
To the men in our lives, it is my fervent prayer that you listen to your body, and have open and frank discussions with your health care providers about when screening is appropriate for you.
Sources:
https://www.everydayhealth.com/columns/health-answers/why-men-dont-go-to-the-doctor/
https://www.cancer.org/latest-news/prostate-cancer-screening-faq.html
https://www.sciencedirect.com/science/article/pii/S1682606X14001133
https://www.usatoday.com/story/news/nation-now/2018/06/04/prostate-cancer-drug-keytruda-shows-positive-results-clinical-trial/668370002/
https://www.pcf.org/c/treatment-options/
View additional resources on CureToday.com
